Eye Motion Content
Activities That Can Change Your Eye Pressure

Activities That Can Change Your Eye Pressure
There have been studies undertaken over the past several years to try and understand if there are any of our day-to-day activities that either help or hurt the management of glaucoma.
Most of the studies demonstrated very little impact on the course of glaucoma. Here are some of the things researches have looked at.
Aerobic exercise: This means doing something at least four times per week for more than 20 minutes at a time that raises your pulse rate to a level that makes your heart work harder. Going from a sedentary lifestyle to active one with aerobic exercise resulted in a very slight decrease in baseline eye pressure.
Yoga: A study conducted at the Mount Sinai Health System (https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0144505) showed a significant increase in eye pressure with any head-down positioning. People with glaucoma would be wise to avoid any exercise that involves a position where your head is lower than your heart.
Weight lifting: Holding your breath while exerting yourself (called the Valsalva maneuver), is also a time when your eye pressure can go sky high. So if you lift weights for exercise, which is generally a good idea to maintain bone density, make it low weights with more repetitions of lifting, rather than heavy weights that make you grunt.
Wind instruments: A similar breath-holding problem applies to those playing the larger wind musical instruments like the French horn. One study suggested that there was a greater chance of glaucoma in symphonic wind players. If you play a brass instrument, it makes sense to have frequent checks of pressure, optic nerve head, and visual field.
Marijuana: Smoking marijuana can lower eye pressure. However, due to its short duration of action (3-4 hours), side effects, and lack of evidence that it alters the course of glaucoma, it is not recommended for glaucoma treatment.
Wearing tight neckties: This creates a very short-duration increase in eye pressure but doesn’t seem to have any long-term effects.
Types of Exams
Routine Examinations
Routine examinations are an overall comprehensive, wellness overview. Each exam includes:
- Visual assessment including a refraction (eyeglasses prescription check, the “better 1 or 2” test)
- Binocular vision assessment to ensure both eyes are working together well.
- Glaucoma screening and risk assessment
- Evaluation of the surface and interior of the eye
- Examination of the internal eye, retina, and optic nerve
- Recommended option to include digital widefield retinal imaging (included with self pay patients, upgrade for insured patients)
If any abnormalities or risks are discovered during your wellness examination, any additional visits and/or testing can be submitted to your medical insurance or may quality for our chronic care package.
In addition to routine examination, we also offer contact lens examinations.
Contact Lens Examinations
Contact lens examinations, in addition to the routine eye exam components, also include:
- Additional evaluation, testing, consultation, and follow-up care related to contact lens wear and performance
- Visual and function assessment of current contact lenses
- Corneal topography to assess the power and contour of the surface of the eye
- Assessment of appropriate positioning and health prospects of contact lens wear
- Assessment of ongoing contact lens candidacy and impact on longterm health of the surface of the eye.
- Consultation and trialing alternative contact lens options, when appropriate.
- Various lens types and prescription needs may require additional consultation and follow-up creating a range of contact lens evaluation fees, from $40 for basic renewals up to $925 for complex corneal disease, post-surgical/graft, orthokeratology fits.
Urgent Eyecare Visits
Our office provides urgent eyecare to those with an immediate need, often with same-day appointments.
- Brief Urgent Care Visits are often for new onset symptoms on the surface of the eye such as pain, discomfort, redness, pink eye, etc.
- Extended Urgent Care Visits usually involve a more extensive analysis of internal eye symptoms such as new onset floaters, flashing lights, new and rapid onset blurred vision. Some of these conditions may need to manage with a tertiary provider in which we will help coordinate care.
Fees & Insurance
Why are healthcare office fees always a great unknown?
This is because insurance plays such a significant role and insurance company details and policies vary greatly. Different rules apply for different insurances, so estimating care costs can be a challenge if not nearly impossible. It's understandably confusing for everyone.
Self insured? Choosing to see us outside of your insurance network? No problem. We believe transparency is essential to earning - and keeping - your trust. We offer a direct care model to individuals without traditional health care or vision discount plans.that are representative of both the quality care we provide and quality support staff we employ. Providing proper value to our patients is a pillar of our patient care goal.
- Routine examinations, including refraction and widefield retinal imaging $172
- Contact lens examinations, also including refraction, corneal topography, and widefield retinal imaging, starting at $220
- Urgent Care Visits, brief $110
- Urgent Care Visits, extended $150+
- Chronic Care Packages are also available for those patients without health insurance who are in need of continual, ongoing care for Dry Eye Disease, Glaucoma, and other eye conditions that necessitate additional testing and ongoing evaluations.
In addition, our private pay self funded patients receive 20% off RX eyeglasses and contact lenses all year for choosing to support our independent practice.
INSURANCE
If utilizing your insurance, our office is contractually bound to upholding and administering that plan according to a patient’s policy. Your costs are determined by your policy and would be consistent office-to-office when in-network.
We work with nearly all major Medical Plans in the area.
IN-NETWORK: Medicare, Anthem BCBS, Aetna, Medical Mutual, United Healthcare, Cigna, Humana, SummaCare
IN-NETWORK BUT RESTRICTIONS APPLY: United Healthcare Optum Care Network, Tricare
NON-PARTICIPATING: Caresource (despite what their Find-A-Provider lists - this is inaccurate), Buckeye, Wellcare, Molina, Paramount
Complicating insurance further, Vision Plans exist to provide routine exam coverage and contribute towards eyeglasses and contact lenses.
IN-NETWORK: VSP Signature, VSP Choice, Eyemed Access, Eyemed Insight, Blue View Vision, Humana Vision
NON-PARTICIPATING: Eyemed Select, Spectera (sometimes marketed as UHC Vision), Davis Vision, Superior Vision, March Vision, NVA (National Vision Administrators)
Insurance is a complicated topic. We strive for and regularly achieve advanced notice of covered and non-covered care, but have been around longer enough to know the rules are constantly changing.
EYEGLASSES
The cost of prescription eyeglasses can vary based on countless factors. There are quality considerations, various optional features and enhancements available, and a wide range of service and support. One pair of prescription eyeglasses from our office can range from $99 to over $1,000.
Our commitment to exceptional service extends to your eyewear as well. Each pair of prescription eyeglasses from our office comes with our professional service for as long as you own them. Refitting adjustments, repairs, replacement nosepads, ultrasonic cleaning are a lifetime inclusion.
Our commitment to quality has us continually evaluating our products offered. We support independent, lens and frame manufacturers also focused on quality and service rather than brand name recognition. We believe your frames should be durable - each frame we offer carries a two-year warranty against defects and breakage. The average frame price in our office is $179.
Similarly to your exam care, vision care plans often determine pricing on prescriptive eyewear. On your own? We offer a 10% Veteran’s Discount and 10% Senior Discount among other revolving promotions.
We feel our fair prices are representative of our superior quality products and expert service continuing long after your purchase. Of course lower-priced eyewear can be obtained elsewhere, however we believe the expression "you get what you pay for" holds true for prescriptive eyewear as well. Providing proper value is always our priority.
| Frames: |
|
| Lenses: |
|
| Add Ons: |
|
Welcome to Eye Doctors of Madison
Welcome to Eye Doctors of Madison
- An Optometric Family Practice
Our practice proudly serves the Northeast Ohio area with a tradition of exceptional service and personal attention.
Michael A. Baker, O.D. takes great pride in offering every patient the absolute best in vision care. He has established our in-office Dry Eye Clinic as well as expanded our Glaucoma Service. Other specialty services include: fitting multifocal contact lenses, managing digital eye strain and computer vision syndrome, and evaluating pediatric patients.
Our expert eye doctor and experienced staff will take the time to answer all of your questions, explain treatment options, and provide the highest quality eye health treatments available.
Built on the foundation of patient convenience and satisfaction, Eye Doctors of Madison serves all of your family’s eye care needs under one roof. Come visit our modern facility and friendly doctors and staff!
Patient Resources and Forms
Patient Portal
Many of our patients find it more convenient to submit their information using our Patient Portal as an alternative to printing out and completing paperwork.
Click the Patient Portal button below to enter information using our Patient Portal, which is directly connected to our office software. This portal is best viewed on a desktop computer.
Patient Portal
New patients: follow link, choose "Let's Start"
Returning patients (previously created a patient portal): enter your info and access code (your Access Code was a password created by you this first time you accessed the password. Please contact our office if you do not remember your access code password.
Patient Forms
For your convenience, and to save you precious minutes during your experience with us, we have provided our office forms below for those who prefer traditional paperwork over online portal access. Click each to download, print, and fill out. Please contact us with any questions you may have.
Essential Forms
History Form and Policies Page
Other office forms for review as needed:
Helpful Handouts
About Us
At Eye Doctors of Madison you will find a caring team of professionals dedicated to providing high-quality personalized eye care for the whole family. We value our patient relationships and strive to improve your quality of life and vision wellness through uncompromised service and state-of-the-art technology. Michael A. Baker, and O.D. and their staff are a close-working team.
Initially established in 1964 by our founder Dr. Nick Donch, O.D., our practice expanded with the addition of Madison’s own Dr. Michael Baker, O.D. in 2009. Dr. Baker’s unique local perspective combined with his extensive training has created a true hometown, family-oriented, environment within our office.
We invite you to refer your friends and family to our comprehensive website and our practice. If you have any questions, please feel free to contact us at our office at (440) 428-2526.
Contact Lens Care Made Easy!

Few things affect the quality of your life more than your eyes--never put them at risk. Contact lenses are prescription medical devices. To make sure your eyes and vision stay healthy while wearing contact lenses, please follow these guidelines or the instructions recommended by your doctor.
Warning: Ocular complications and/or long-term corneal damage are the consequences of contact lenses that are worn longer than recommended. Oftentimes, your lenses will still feel fine even when you are over-wearing them. Do not wear your lenses overnight unless they are approved for extended wear and your doctor has discussed this with you. Overnight wear increases the risk of infection and other complications.
Wearing Schedule
It will take at least a few days for your eyes to get used to wearing contact lenses. The best way to insure maximum visual comfort and keep your eyes healthy is to patiently and faithfully adhere to this wearing schedule.
| Day | Gas Permeable Lenses | Soft Lenses |
|---|---|---|
| 1 | 4 hours | 6 hours |
| 2 | 6 hours | 8 hours |
| 3 | 8 hours | 10 hours |
| 4 | 10 hours | 12 hours |
| 5 | 12 hours | 12 hours |
- DON’T wear your lenses longer than 12 hours a day until your first follow-up visit with your doctor, unless the doctor has specifically told you otherwise.
- DON’T continue use of contact lenses if your eyes become red, irritated, painful, or if your vision gets worse while wearing lenses. Immediately take out the lenses and clean them. Let your eyes get back to normal and if the problem persists, contact our office.
- DON’T exceed the wearing times suggested, even if your lenses still feel comfortable. Studies have proven that the eye needs time to adapt to contact lenses, and your wearing schedule is based on those studies.
- DO always remove your contact lenses at least one hour before going to bed to allow for proper oxygen nourishment to the cornea.
- DO schedule and keep follow-up appointments with your eye doctor.
- DO wear your contact lenses for at least 4 hours the day of your follow-up appointment unless you are experiencing discomfort.
Please Note: If you complete your wearing schedule for a given day and take out your lenses for at least 2 hours, you can wear them the same day for another 2 to 3 hours after cleaning and disinfecting them.
Caring For Your Contacts
Deposits and infectious organisms, such as bacteria and viruses, can build up on the surface of all contact lenses. For this reason, it is very important to keep them clean and disinfected.
 There are four steps in contact lens care--follow the care prescribed for your lenses:
There are four steps in contact lens care--follow the care prescribed for your lenses:
- Cleaning removes dirt, mucous, and other debris that gets on the lenses during wear.
- Disinfecting kills bacteria (germs) on the lenses. Disinfecting is essential to prevent serious eye infections.
- Rinsing removes the other solutions from the lenses and prepares the lenses for wear.
- Enzyming uses enzyme drops or tablets to remove protein and other deposits that build up over time on the lenses.
The best way to properly care for your lenses is to develop a care routine, then stick to that routine! Remember to:
- Follow the directions outlined by your eye doctor. Oftentimes instructions are also listed on the packaging or the package insert for the contact lens solutions prescribed for you.
- Multi-purpose solutions can be used for more than one step in contact lens care. Read the label to see which functions the solutions can be used for.
- Many solutions can not be used together, and not all solutions are appropriate for all types of lenses. Only use solutions recommended by your eye doctor, and check with your eye doctor if you want to switch brands.
- When you remove your lenses, they must be cleaned, rinsed, and disinfected before they are worn again.
- Enzyming and cleaning are not a substitute for disinfecting.
- Lenses that have been stored for more than 12 hours may need to be cleaned, disinfected, and rinsed again.
- Make sure solution containers are kept closed tightly, stored upright, and kept in a clean, dry, cool place when you are not using them. Keep your case clean and replace it every 2-3 months to prevent bacterial growth.
- Don’t touch container bottle tips to any surface to prevent them from becoming contaminated.
- Throw away expired solutions. (Look on the bottle for the expiration date!)
- Use new solution in your contact lenses case every day.
- Discuss with your eye doctor the care for your lenses if you wear them while swimming in a pool or hot tub.
- Only use approved rewetting drops for lubricating or wetting your lenses. Never place the lenses in your mouth.
- Do not use tap water to rinse soft contact lenses.
- Be careful with makeup, lotions, creams and sprays--consider putting on lenses before makeup and remove them before removing makeup. Also, water-based makeup is less likely to damage lenses than oil-based makeup.
Here’s what you need to watch for: redness, blurriness, light sensitivity. Remove your lenses if you are experiencing any of these 3 things. If your eyes have not returned to normal after 24 hours, please contact our office. If you have any change in vision, comfort, or irritation, immediately remove your lenses. If there is no improvement within a couple of hours, please contact our office.
Video Learning Center
Welcome to the Eye Doctors of Madison video learning center! Please call our office at (440) 428-2526 if you have any questions about the conditions you see here.
Contact Us
At Eye Doctors of Madison, our professional eye care staff will be happy to assist you with your vision needs. We have treatment options available for everyone. Whether you are interested in making an appointment for a LASIK consultation, have cataracts, need an annual eye exam, or just need glasses, we can help!
Contact us today to begin scheduling an appointment using the form below, or call us directly at (440) 428-2526. If you need to order contacts, you can reach us through the form below, or order contacts directly here.
Blog
We'd like to welcome you to our newly minted website. We have taken great care to ensure this site keeps you better informed about Eye Doctors of Madison and to provide relevant information in an easy to understand way.
Please vist our page often as we will be updating with specials and promotions throughout the year. While you are here please take time to visit our Video Learning center, in the Eye Health drop down, where you can view our entire library of eye related videos.
Community Outreach
It is my belief that no child should go without proper eye care, regardless of socioeconomic or insurance status. As a fellow Madison-schools parent as well as Madison High School alumnus myself, the ability to give back to my community is a blessing. My office provides reduced or no cost eye care and eyewear to Madison Local Schools students for those students and families who demonstrate need.
Dr. Michael Baker, O.D.
2001 Madison High School Graduate
VOS: Vision Outreach for Students
Our community support program has one simple goal: provide any Madison child with a needed eye exam and prescription eyeglasses. Any Madison who simply has the need is able to apply.
Eligible individuals include:
- Madison local schools student
- Demonstrable need of financial hardship.
Our office hosts clinics several times throughout the year specifically for this program. Please see this attached document for program details and policies.
For some individuals, eyeglasses materials may be provided in partnership with the Essilor Vision Foundation’s ‘Changing Life Through Lenses” program for individuals at or below the federal poverty level. We would like to thank the EVF for their support with our local initiative.
If you are interested in this program and would like to check on eligibility for you or a child, please fill out the form below.
Appointment Information
We know you have endless options for eye care providers but we could not be more excited to welcome you to Eye Doctors of Madison. Here are a few things to keep in mind about your upcoming appointment:
- Bring in all prescription eyewear (glasses, sunglasses, computer glasses, contact lenses, etc.). Knowing your current products will best allow Dr. Michael A. Baker, O.D. to determine any changes, make recommendations, and customize your vision to suit your needs.
- Bring a photo ID and ALL insurance cards with you to your appointment, both medical insurance and vision care plans.
- Please peruse our Patient Portal prior to your visit. This will allow you to complete or update your general health information and review our office procedures and policies in advance.
- For new patients not utilizing our Patient Portal, we encourage you to complete and review paperwork in our “Essential” Office Forms section.
- We know your time is valuable, so we ask that you arrive NO EARLIER than 10 minutes to your appointment. To be fair - we schedule appointments to dedicate proper time to each and every patient. Patients are seen in the order they are scheduled. You may call us to inquire about early arrival, sometimes we may be able to accommodate early arrivals due to last minute cancellations.
- If you are unable to make your appointment at your scheduled time, please call or email us PRIOR to your scheduled appointment time to allow us the opportunity to allow others to fill your allocated time.
- We're easy to find - but here are directions just in case!
- We're easy to reach - call, email & even messenger!
We are LOOKing forward to SEEing you!
Products Overview

When it comes to vision care products, they are not all created equally! Across the eye care industry there is a large variance in quality and craftsmanship. We take pride in using a wide-range of top quality materials with great product support to provide you with the excellent eye care products. We meet regularly with manufacturer's representatives to make sure that we have the a great selection. Our value is in knowing what is available and what best meets your needs.
When considering where to purchase your eyeglasses, contact lenses, and sunwear, remember to consider the following. . .
Total Eye Health - Our office is part of this community. We want you to have sharp vision and great comfort with your glasses and contact lenses. The health of your eyes is our major concern. That is why we stand behind our products and services with great warranties, and a professional and well-educated team. Different prescriptions require certain frame styles and lens treatments in order for your glasses to perform well and look great. Our trained opticians can guide you through this process. Our dispensary has hundreds of frames from which to choose, including a large selection of children's frames. We can help you find the size, shape, and color of frame that is perfect for all family members. When it comes to contact lenses, we offer a full spectrum of products. Even if you have been told before that you cannot wear lenses, we may have a solution that is right for you.
Competitive Pricing - At Eye Doctors of Madison we offer competitive pricing, affordable eyewear packages, and multiple-pair savings. You are also welcome to take advantage of manufacturer rebate programs and special promotions through our office. Be sure to ask about our convenient contact lens direct shipping program.
Convenience - Your Eye Doctors of Madison offers a wide selection of products in our office as well as through custom orders. We use great quality materials and will courteously recommend eyewear and contact lenses that fit your lifestyle and fashion - all within your budget. Plus, you get to try on your frames before ordering--instead of just ordering online and hoping they work for your face and your prescription!
Lenses & Coatings
Contacts & Solutions
Sport & Sunwear
Bifocal Lenses

For many people, different lenses are needed for seeing at different distances. Bifocal lenses allow the wearer to look through two areas of the lens. One area focuses on distant objects. The other is used for reading. A little-known fact is that bifocals were invented by Benjamin Franklin, and his style of bifocals are still available today.
Most of the time the “reading” area is smaller, shaped like a sideways “D”, and found in the lower hemisphere of the lens. These bifocals are called line bifocals or flat-tops. If you are focusing on distant objects, you look through the top half of the lenses. To read a book, magazine, or newspaper, you look through the “reading” area. The Franklin style lenses are less common, and are split horizontally down the middle of each lens. One thing that is difficult about using bifocals is dealing with the line between the two vision areas. Fortunately, recent technologies have developed a new type of lens, called the no-line, or progressive, lens.
Progressive Lenses

One of the main problems with bifocal and trifocal lenses is the issue of eye fatigue. It can be difficult to switch from one focusing power to another. Your eyes can tire, which can even lead to a headache, sore neck and sore back.
A variation of bifocals and trifocals is the no-line lens or progressive lens. No-lines provide a smooth transition from focusing on nearby to distant objects because they do not have a distinct line separating the focusing powers. Instead, a gradual change in power allows the wearer to focus on objects at all distances. Distant objects are viewed through the upper portion of the lens, while near objects are viewed through the middle or lower portion of the lens. These are also great for computer users.
Trifocal Lenses
Bifocals allow the wearer to read through one area of the lens, and to focus on distant objects through another area of the lens. As the eyes age, though, a stronger prescription is often needed to read. This would be fine, but the stronger prescription that allows for reading makes it difficult to focus on objects at intermediate distances, such as grocery items on a shelf or your speedometer. Thus, trifocals are necessary for a third prescription for intermediate focusing.
Trifocals, also known as line trifocals, feature three areas of focusing power, each separated from the other by a distinct line. The three windows allow for focusing on distant objects, intermediately distanced objects, and for reading. The downside of trifocals is dealing with the lines between the different focusing powers. Fortunately, recent advances in technology have led to developments in no-line, or progressive lenses.
High Index Lenses
Previous to the last few years, the only materials available for use as lenses were glass and a hard resin called CR-39. But recently, high index lenses have become available. High index materials are named because they have a higher index of light refraction. Basically, they can do the same job that glass or CR-39 does, but high index lenses are much thinner and lighter. With high index lenses, you can avoid having “soda bottle” lenses.
When learning about high index lenses, you may hear many unfamiliar numbers and terms. Here are a few things to remember.
Polycarbonate
The first and still the most popular high index plastic is polycarbonate. Polycarbonate was originally developed for fighter jet cockpits. It is very strong, very light, and resistant to scratches and breaking. Most sports lenses are made of polycarbonate.
Mid-Index
Other high index materials are classified by numbers. The higher the number, the thinner and lighter the lens. The lower numbers are classified as mid-index lenses. Mid-index lenses, such as 1.54, 1.56, and 1.57, are thinner than glass, and nearly as strong as CR-39.
High-Index
High index lense are much thinner than regular glass or plastic. Talk with your doctor to decide which high index lens is right for you.
Anti-Reflective Coating

Normal eyewear often creates glare, reflections, and “ghost images.” Now all that can be eliminated with an anti-reflective coating.
What we see is a result of light being sensed by our eyes. With normal glasses, much of the light reflects off the lenses. This produces glare. It also reduces the wearer’s visual acuity. In other words, the light reflection is both a cosmetic and visual problem.
Anti-reflective coatings increase light transmission through the lenses to 99.5 percent. They make it easier to see and easier for others to see you. These coatings are especially useful for those viewing computer screens and driving at night.
Polarized Lenses

Glare from wet roads, light reflecting off other vehicles, and glare from your own windshield can be annoying and dangerous. To eliminate this glare, we offer polarized lenses. Polarized lenses eliminate the majority of glare, reducing eye strain and increasing visibility. Polarized lenses are the most effective means to reduce glare.
Most glare comes from horizontal surfaces, so the light is “horizontally polarized.” Polarized lenses feature vertically-oriented “polarizers.” These polarizers block the horizontally-polarized light. The result is a glare-reduced view of the world. Polarized lenses can make a world of difference for any outdoor enthusiast. Fisherman can eliminate the bright reflections from the water and actually see into the water more easily than with other sunglasses, golfers can see the green easier, and joggers and bikers can enjoy reduced glare from the road. In addition, drivers can enjoy the safety and comfort that polarized lenses provide while driving.
Scratch Resistant Coating

If you have hard resin lenses (CR-39), you should consider getting a scratch-resistant coating. Resins and plastics are more susceptible to scratches than glass. Scratches damage the cosmetic look of the lenses and compromise their performance. With a scratch-resistant coating, you do not have to worry as much about minor scratches on your lenses.
Another advantage of scratch-resistant coatings is that most coatings come with a one-year warranty. They are a great investment to prevent minor scratches. However, it is important to remember that scratch-resistant does not mean scratch-proof. All lenses are susceptible to scratches.
Photochromics
If you have ever felt frustrated at needing both prescription glasses and prescription sunglasses to accommodate an outdoor lifestyle, you should consider photochromic lenses. Photochromic lenses darken when exposed to UV rays. The change is caused by photochromic molecules that are incorporated into the lens or into a coating on the lens. When the wearer goes outside when it's bright, the lenses darken automatically. When the wearer goes back inside, the glasses become clear.
There are a variety of photochromic options available. Depending on what you choose, you can customize the lenses to your needs. Some lenses darken only in direct sunlight, while others darken in little or no direct light. Some are designed to darken while you are in the car to reduce road glare while you are driving. You can even choose the color of the tint. Ask your doctor what options are available.
Cosmetic and Specialty Tints
Your glasses do not have to be an eyesore to those around you. Eyeglasses can be a stylish accessory, a part of your personality, or a way for you to be unique. There are a variety of frames to choose from, but you may not know that there are also many ways to improve the appearance of the lenses. Cosmetic tints are now available. These tints offer a variety of colors and shades. You can choose light blue or any other color of the rainbow. Some lenses are clear at the bottom and gradually get more colored towards the top of the lenses. There are many ways to adjust your lenses to whatever style suits your personality. Some tints are also functional.
Recently there has been much attention on a condition called Computer Vision Syndrome, or CVS. A special tint for your glasses can reduce eyestrain associated with CVS.
Specialty Lenses

We all have heard the phrase, “Different strokes for different folks.” Well, this also holds true when it comes to selecting glasses. There are different lenses for just about everybody. No matter what your particular need, there is probably a specialty lens designed for you.
For example, a specialty lens that is becoming increasingly common is one designed for computer users. Computer lenses have “windows” designed for viewing your computer screen, documents on your desk, and distant objects. The lenses are designed to reduce Computer Vision Syndrome, or CVS, which is characterized by headaches, eye strain, neck and back aches, dry eyes, blurred vision, and double vision.
Another example is called the double D-segment lens, also known as the double flat-top lens. If you look through most of the lens, you can focus on distant objects. But you can also look through a D-shaped segment near the top of the lens to see nearby overhead objects more clearly. This is very useful if you are involved in work where you are looking at nearby objects above your field of vision, as with carpenters and pilots. The D-shaped segment near the bottom of the lens allows for reading.
Contacts & Solutions

Contact lenses, when used properly, are very convenient, and with the latest advancements in technology, they are extremely comfortable. Most of the time, you will hardly know you are wearing them, though you will certainly notice how clear and accurate your vision is. Contact lenses are small lenses worn on the surface of the eye, or cornea, to correct vision. Lenses are sometimes worn for cosmetic purposes only. We recommend wearing contact lenses in conjunction with eye glasses. This allows you to best meet your overall lifestyle needs while protecting the integrity of your overall eye health.
We will discuss the option that is best for you. Many patients choose contact lenses for their primary vision correction and glasses as a backup option. Many patients who wear glasses have activities and events where they would rather not wear their glasses and they choose contact lenses for these times.
Contact Lens Types
The types of contact lenses available have exploded in the past few years. There are contact lenses available for almost everyone. Many or our patients were told in the past that they could not wear contacts, or they tried unsuccessfully to wear contact lenses. You owe it to yourself to see what is new. We carry many options, and promise to do our best in selecting contact lenses that you will love wearing. Choose from the following list for a brief look at some of the options available.
Disposable Soft Lenses
Disposable soft lenses are much more popular than conventional soft lenses. These lenses are worn for a period of time and then, of course, thrown away. Disposables may be designed to last for one day or up to a couple weeks. These are perfect for many patients who were told they could not wear contact lenses because of allergies or mild dry eye conditions. They have a low cost per lens and are also popular for athletes and hobbyists who do not necessarily want to wear contact lenses every day.
Soft Colored Contact Lenses

Interested in a new look? Then tinted lenses might be a good fit! These soft lenses are available in conventional, disposable, or frequent replacement types. With tinted soft lenses, you can change or enhance your eye color. Even if you do not need corrective lenses, you can use “plano” colored contacts to change your eye color. It is important to be fitted by an eye doctor for colored contact lenses even if you do not need a prescription; wearing the wrong style can damage your eyeball.
Bifocal Soft Lenses
Recent technology has greatly improved bifocal soft lenses. Many patients past their 40s who need bifocals can now enjoy the comfort and benefits of soft contact lenses. Ask your doctor to see if this would be a good fit for you.
Toric Soft Lenses
Toric lenses are used to correct astigmatism. Astigmatism is a vision condition where an irregularly shaped cornea affects the vision. In the past, the only options for those with astigmatism were either glasses or hard gas permeable contact lenses. But toric lenses, which are lenses with a special shape, now offer an alternative. There are several types of toric lenses to choose from.
Extended Wear Soft Lenses
Extended wear lenses, the result of new technology in lens materials, transmit more oxygen to the cornea of the eye. Some of these lens materials can be worn up to 30 days, day and night, without removal. Extended wear lenses can last one week, two weeks, or one month, depending upon the lens material and your doctor’s recommendations.
Rigid Gas Permeable (RGP) Lenses
As the name implies, these lenses are hard and gas permeable. If you’ve been told you cannot wear soft lenses, RGP lenses are often a great alternative. RGP lenses are available in specialized designs to correct just about any vision disorder.
Solutions

There are a variety of solutions available from many different manufacturers. The important thing to remember is that not every solution is right for every type of contact lens. Some contact lenses require the use of multipurpose solutions, while others require separate solutions for the four steps in contact lens care: disinfecting, cleaning, rinsing, and enzyming. Use only the lens solutions that are recommended by the eye doctor. If you wish to change brands, check with our office first.
Sports Lenses

If you play sports, you should keep two things in mind related to your vision: protection and precision.
Sports lenses protect the wearer’s eyes. Sports such as tennis, baseball, softball, and racquetball may see ball speeds of 90 mph or more. In baseball alone, there are over 500,000 injuries per year! But that is not the most common cause of sports-related eye injuries. Most eye injuries occur in basketball, where an elbow or a finger jabbed into the eye can cause corneal abrasions, fractured bones, retinal detachments, or even blindness. Polycarbonate lenses are more resistant to impact than glass or plastic and offer protection for 90% of eye injuries. Protective eyewear fits well, features a padded bridge, has prescription or non-prescription lenses, and has deep-grooved eyewires to prevent the lens from falling out.
The specialized lenses also optimize your vision. Depending on your sport, certain lenses are more appropriate than others. Dark, UV protection lenses are great for baseball and other outdoor sports. Golfers can benefit from gray-brown colored lenses which make it easier to outline the course. Even if you do not normally wear glasses, non-prescription sports lenses can benefit your performance. Some people think that lenses prevent the wearer from seeing the action, but many sports lenses have anti-fog, glare reduction, and scratch resistant properties. Some are also designed to maximize peripheral vision.
Sunwear

To reduce exposure to UV rays and their effects, we recommend you invest in a set of sunglasses which can provide at least 98% protection from UVA and UVB rays. While cheaper sunglasses can range from poor to excellent UV protection, our sunwear lines provide top quality protection from the sun. We carry a large selection of styles and colors.
Another product to consider is a pair of polarized sunglasses. Polarized lenses block light reflected from surfaces such as a flat road or smooth water. If you are involved in activities such as water sports, skiing, golfing, biking, fishing, and even driving, polarized lenses can be very helpful in reducing glare and giving a clearer view.
Finally, if you have a youngster in the family, it is never too early to fit them with sunglasses. Children under the age of 20 are the most susceptible to the damaging effects of UV light. One concern of parents is that their child will scratch, break, or lose the sunglasses; we are here to help you make the best choice for your child.
Eye Anatomy

Don’t remember the lessons on eye anatomy from your highschool biology class? That’s OK—we have provided the following eyeball illustration and terms just to give you a refresher course. And we won’t give you a pop quiz afterwards…
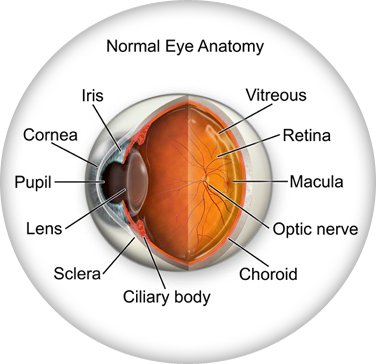
| IRIS | Pigmented tissue lying behind cornea that (1) gives color to the eye, and (2) controls amount of light entering the eye by varying size of black pupillary opening; separates the anterior chamber from the posterior chamber. |
| CORNEA | Transparent front segment of the eye that covers iris, pupil, and anterior chamber, and provides most of an eye's optical power. |
| PUPIL | Variable-sized, circular opening in center of iris; it appears as a black circle and it regulates the amount of light that enters the eye. |
| LENS | Natural lens of eye; transparent intraocular tissue that helps bring rays of light to focus on the retina. |
| SCLERA | The white of the eye; a protective fibrous outer layer covers all of the eyeball except for the part covered by the cornea |
| CILIARY BODY | a muscular ring under the surface of the eyeball; helps the eye focus by changing the len’s shape and also produces aqueous humor |
| CHOROID | The vascular layer between the sclera and the retina; the blood vessels in the choroid help provide oxygen and nutrients to the eye |
| OPTIC NERVE | Largest sensory nerve of the eye; carries impulses for sight from retina to brain |
| MACULA | Small, specialized central area of the retina responsible for acute central vision |
| RETINA | Part of the eye that converts images into electrical impulses sent along the optic nerve for transmission back to the brain. Consists of many named layers that include rods and cones |
| VITREOUS | Transparent, colorless, gelatinous mass; fills rear two-thirds of the interior of the eyeball, between the lens and the retina |
Vision Conditions
Select from the following list or scroll to learn more about the symptoms and treatments for:
Emmetropia
When rays are focused correctly on the retina of a relaxed eye, the eye is said to be emmetropic. Emmetropia is the medical term for 20/20 vision, vision that needs no corrective lenses, contact lenses, or reading glasses. It occurs because the optical power of the eye can perfectly focus an image to the retina, giving it “perfect” vision.
The opposite of emmetropia is ametropia. With ametropia, the focal point of the eye is some distance in front of or behind the retina. The following vision conditions are types of ametropia.
Hyperopia and Myopia
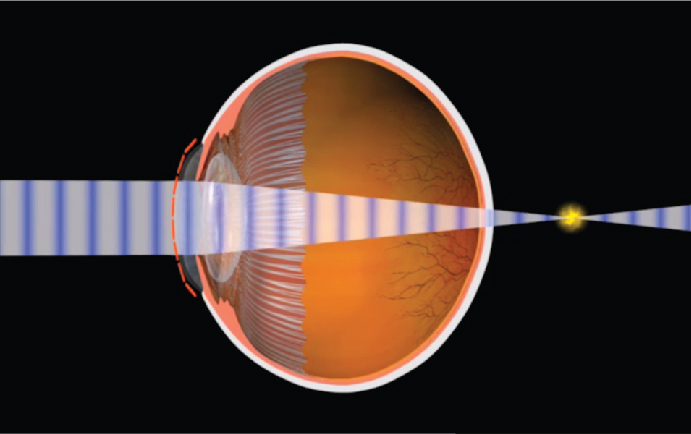
Hyperopia
Hyperopia is more commonly known as farsightedness. As the name suggests, people with farsightedness are able to focus on objects that are further away, but have difficulty focusing on objects which are very close. This is because the eyeball is shorter than normal, which prevents the crystalline lens in the eye from focusing correctly on the retina. About a fourth of the population is farsighted. Hyperopia can lead to chronic glaucoma, a more serious condition, later in life.
A family history of hyperopia is a risk factor for developing hyperopia. Babies are often born with hyperopia but they can usually outgrow the condition as their eyes develop into the correct shape.
Hyperopia can be corrected with eyeglasses or contact lenses. There are also new surgical procedures that can correct hyperopia.
Myopia
Myopia is the condition of being nearsighted. When it is an inherited condition, myopia begins early in life. People with this condition can usually see near objects, but they struggle to see distant objects. Myopia is the opposite of hyperopia, or farsightedness. In myopia, the anatomy of the eyeball, or globe, is longer than normal. This causes the light to focus in front of the retina, blurring the distance vision. Myopia is corrected with glasses and contact lenses, or with laser vision correction. Laser vision correction is only recommended for people over 18 years old, when the eye has finished growing to adult size.
To correct the symptoms of myopia with glasses, lenses are used that are thicker on the edges and thinner in the middle. This is known as a concave lens, which can be cosmetically improved in higher prescriptions with a high index lens.
Myopes are also at increased risk for a retinal detachment. The signs and symptoms of a retinal detachment are flashing lights, black floaters, or a curtain over the vision. The risk of detachment is typically less than 3 percent.
Amblyopia

Amblyopia defined
Amblyopia is also known as lazy eye. It is a condition, usually found in children, in which one or both eyes do not develop properly. An easy way to explain this is that the "eye-brain" connection does not communicate properly; therefore, the child does not know what clear vision is...or what 20/20 vision is. The eye anatomy itself is normal, but the neural pathway to the brain is not normal, causing decreased vision.
Prevalence of amblyopia
Amblyopia is one of the most common treatable forms of vision impairment in children. Its prevalence is as high as 3-5% in some studies. It is most common in infants and young children and it is imperative that this condition is caught early. The chance of successful vision restoration goes down dramatically after age 8, therefore the earlier this condition is caught the better chance of successful treatment.
Causes of amblyopia
The causes of amblyopia are varied. A very common condition that can cause amblyopia is strabismus, a misalignment of the eyes. This occurs when one eye has an abnormal turning in or out, causing the brain to stop using the misaligned eye. Other causes may come from a high prescription such as nearsightedness, farsightedness, or astigmatism. In the case of these conditions, the eye’s vision is out of focus and so the brain turns off that image. Eye disease processes can also cause amblyopia. One of these conditions is known as a cataract. A cataract is a condition of the lens of the eye developing an opacity so that light cannot pass through. Abnormal retinal conditions and hereditary factors can also cause amblyopia.
Treatment of amblyopia
 In order to increase the chances for success, this condition must be detected early. The recommended ages for early eye examination are 6 months old, then 2-3 years of age, and then school age.
In order to increase the chances for success, this condition must be detected early. The recommended ages for early eye examination are 6 months old, then 2-3 years of age, and then school age.
Patching, or occlusion therapy
One of the most common treatments for amblyopia is patching, also known as occluding, the better or stronger eye. This forces the brain to use the weaker eye. An adhesive eyepatch on the skin or a slip-on patch over glasses can be incorporated for occlusion therapy. A blurring contact lens or dilating eye drop can also be used to occlude the good eye.
Surgery
Cataract, eye muscle, or retinal surgery can be incorporated to help treat the underlying cause of amblyopia in some cases.
Vision therapy
Vision therapy has been proven to be successful in the treatment of amblyopia. Vision therapy, or VT, incorporates a series of vision training procedures that helps improve eye movement control, visual acuity, depth perception, and eye coordination. Vision therapy can be done in an office or home setting.
Signs and symptoms of Amblyopia
The most common way amblyopia is diagnosed is a detection of a decreased red reflex in the child's eye. A diagnostic instrument used by the optometrist, ophthalmologist, or pediatrician, can pick up a bright reflection in the normal eye and a dim reflection in the amblyopic eye. Upon further examination, the eye is dilated to see if a refractive error of myopia, astigmatism, or hyperopia is the cause.
Another sign of amblyopia is an eye that turns in or out. A symptom that may be indicative for amblyopia is if the child prefers the vision out of one eye. This can sometimes be detected when occluding the better eye--the child may become fussy and upset because she cannot see out of the lazy eye.
Citations:
1. Amblyopia informational patient brochure. APOS.org. January 2013
Presbyopia

As people get older, usually when they hit their 40s, a condition called presbyopia can set in. Presbyopia is the inability to focus on objects near the eye. One usually notices that it is harder to read or use the computer. Bifocals or reading glasses are a way to remedy this condition.
Presbyopia is a natural consequence of the aging process. There is no known cure, though researchers are constantly looking for one. Even if someone has never had vision problems before, he can still develop presbyopia. It may seem to occur suddenly, but it actually occurs over a long period of time. Symptoms include having to hold things at arm’s length to see them clearly, eye strain, fatigue, and headaches from near work.
Astigmatism
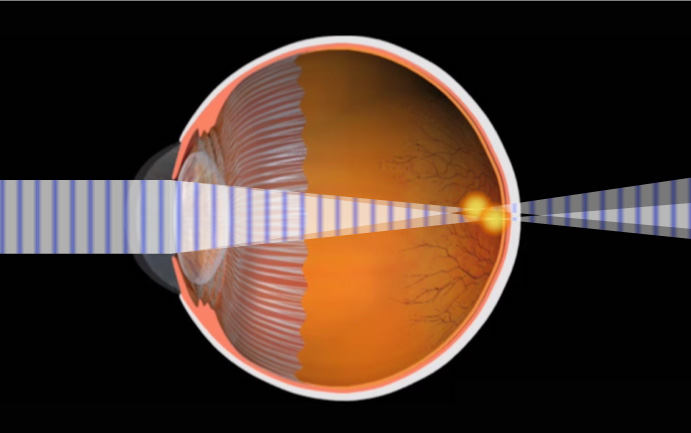
Sometimes the cornea is irregularly shaped, causing the eye to focus an object on two different areas of the retina. This is known as astigmatism. For the cornea to bend light correctly, it should be dome-shaped, like a basketball. Astigmatic corneas are shaped more like a football. This causes a distorted view when looking at objects which are close-up and far away.
The cause of astigmatism is unknown. Astigmatism is often associated with myopia or hyperopia, and it usually is present from birth. It may be hereditary, or it may be caused by factors such as pressure on the cornea, incorrect posture, or increased use of the eyes for “near work.”
Mild astigmatism usually does not need to be corrected. Eyeglasses, contact lenses, or refractive surgery can correct moderate to high degrees of astigmatism.
Computer Vision Syndrome

Computer vision syndrome (CVS) affects three out of four computer users. It is a series of symptoms related to extended periods of computer usage. Though it is no cause for panic, measures can be taken to relieve symptoms of CVS.
Symptoms
CVS can appear as a variety of symptoms. Headaches, eye strain, neck and back aches, sensitivity to light, blurred vision, double vision, and dry or irritated eyes are all possible problems related to CVS.
Risk Factors
Any computer user can develop CVS. Your vision, your computer, and the environment where you use your computer are all factors which can lead to CVS.
Diseases of the Eye
Our top priority is the care of your eyes. We want to keep your eyes healthy through regular eye health evaluations, communication, and education. This page lists a few of the most common eye diseases. Select from the following list of topics or scroll to learn about the causes, symptoms, and treatments for:
Blepharitis

There are two types of blepharitis. Seborrheic blepharitis is often part of an overall skin condition called seborrhea, which may also affect the scalp, chest, back and the area behind the ears. The second form of blepharitis – staph blepharitis – is a more severe condition, caused by bacteria, that begins in childhood and may continue through adulthood.
Causes
Hormones, nutrition, general physical condition, and even stress may contribute to seborrheic blepharitis. Build-ups of naturally occurring bacteria contribute to staph blepharitis.
Symptoms
Blepharitis could be described as dandruff of the eyelids. Seborrheic blepharitis results in redness of the eyelids, flaking and scaling of eyelashes, and greasy, waxy scales caused by abnormal tear production. Staph blepharitis can cause small ulcers, loss of eyelashes, eyelid scarring, and even red eye.
Treatment
Careful cleaning of the eyelids can reduce seborrheic blepharitis. Application of hot packs to the eyes for 20 minutes a day can also help. Staph blepharitis may require antibiotic drops and ointments.
Cataracts
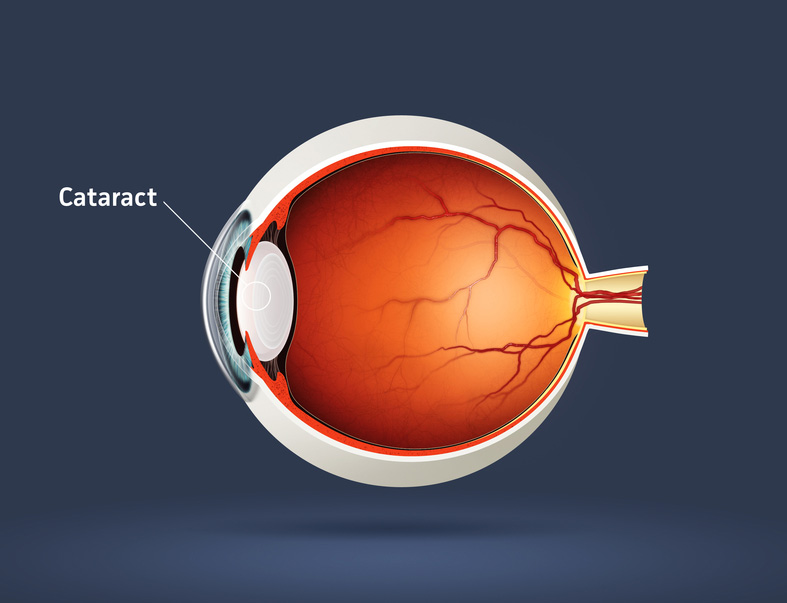
A cataract is an opacity of the lens of the eye. The body's natural lens is similar to an onion, with many layers. These layers contain protein and as the proteins clump together, they cover the lens and make it difficult to see clearly. Cataracts are generally seen in the older population, but they can occur at any age, even birth. By age 60, over half of the population has some symptoms of cataracts due to the natural aging process.
Cataracts are painless but if left untreated can lead to blindness. Cataract surgery is done on an outpatient basis with little or no downtime afterwards. The surgery is performed by a medical doctor known as an ophthalmologist, who specializes in surgery of the eye. The aftercare or postoperative care can be administered by an ophthalmologist or an optometrist.
Symptoms of Cataracts
There can be a myriad of symptoms when a person develops a cataract. It is common for vision to be blurry, as though you are looking through a foggy window. Color vision changes occur in which the brightness of colors fade, especially blue and green. Patients with cataracts also experience difficulty in reading small print. They also feel like they need brighter light or possibly a new glasses prescription. Double vision or vision that seems like halos around the letters also occurs, as well as sensitivity to light.
Causes of Cataracts
The exact physiological cause of cataracts is unknown, but there are many risk factors. Aging and trauma are known to cause cataracts. A blunt trauma or injury to the eye can cause a cataract at any age. The effect of aging on the cells of the lens contributes to cataracts usually after age 60. There is also a direct correlation between the sun's UV rays and certain radiation exposures that contriibute to cataract growth. Smoking is a big risk factor for developing cataracts as well.
Poor nutrition can add to the risk of developing cataracts. Lack of vitamin C has been shown to increase the genesis of cataract formation. Some prescription medicines, especially prednisone, can cause cataracts. Diabetes and other chronic disease processes are also factors in cataract formation. Finally, there are genetic factors that contribute to a cataract.
Treatment of Cataracts
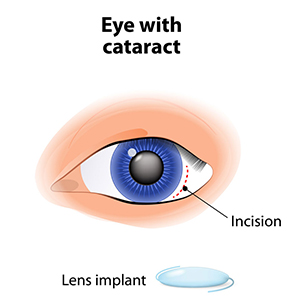
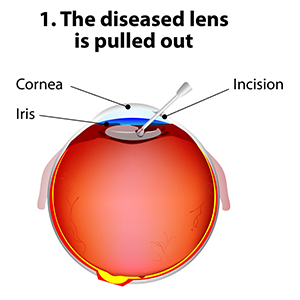
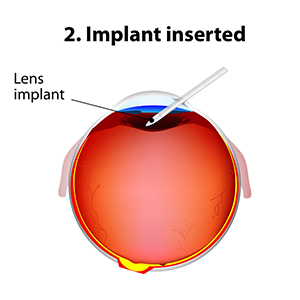
The standard of care for the treatment of cataracts is typically surgery. Cataract surgery, which is an outpatient procedure, removes the protein accumulation from the eye by replacing the cloudy natural lens with an artificial lens. This artificial lens, known as an IOL or intraocular lens, will have your prescription, which in most cases, makes you less dependent on glasses. Lens technology has evolved over the years to also accommodate prescriptions for astigmatism and bifocal prescriptions. Cataract surgery is one of the most commonly performed surgeries in the United States, and it has a success rate of over 98%.
There are many types of cataracts that form on the eye, with different levels of density. This can affect the post-operative care of cataract patients. After cataract surgery, it might be necessary to use a laser to clear an after-cataract membrane that can occur weeks to months after the procedure. This treatment uses a YAG laser and is a painless, low risk, in-office procedure. Most patients can return to work or normal activities within days after the procedure. Your doctor will likely prescribe eyedrops to prevent infection and swelling.
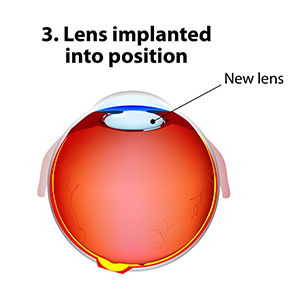
Recent Findings
New technology in cataract surgery includes a bladeless customized procedure that allows for faster healing and clearer vision after the procedure. This computer assisted surgery uses a laser to make the incisions. The laser also divides the cataract efficiently so that the surgeon can remove the old lens and replace it with a new state-of-the-art IOL ( Intraocular lens). This technology uses a femtosecond laser which emits cool pulses of energy. This technology has been used for decades in LASIK surgery for the correction of myopia or nearsightedness. This form of cataract surgery now allows the procedure to be more precise, and reproducible.
Citations
1. What is a cataract? Educational website release. Triadeye.com. January 13, 2013.
2.Bladeless cataract laser surgery. LenSX press release. October 4, 2012.
Conjunctivitis

Conjunctivitis, commonly called pink eye, is a redness of the eye. It is often accompanied by a discharge (clear, yellow, or white) and itching in the eye.
Causes
Pink eye is most often a viral infection, but it can also be caused by bacteria or an allergic reaction. Viral pink eye is highly contagious.
Prevention and Treatment
To avoid spreading conjunctivitis, wash your hands often, do not touch the infected area with your hands, do not share washcloths or towels, and avoid using makeup which may become contaminated. A child with pink eye should be kept from school for a few days. Sometimes an eye doctor will need to prescribe antibiotic eye drops and ointments to clear up conjunctivitis.
Diabetic Retinopathy
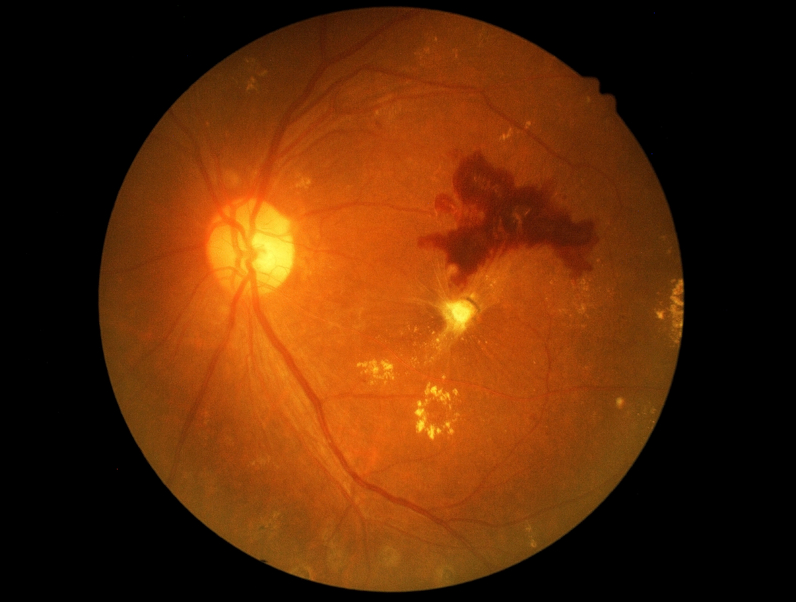
Diabetic retinopathy is a condition associated with diabetes. High levels of blood sugar may damage tiny blood vessels in your eye. New vessels may form to replace the damaged vessels. The new vessels can burst, resulting in blurred vision or even blindness.
Symptoms
Symptoms of diabetic retinopathy include:
- "Floaters” – small specks that pass across your field of vision, made up of cells floating in the transparent gel of your eyeball
- Difficulty reading or seeing things close-up
- Sudden loss of vision
- Flashes
- Blurred or darkened vision
Risk Factors and Treatment
If you have diabetes, make sure you control your blood sugar level. This will reduce your risk of getting diabetic retinopathy. If you are experiencing some of the symptoms listed above, give us a call. If diagnosed properly, diabetic retinopathy can be treated with a laser procedure or a vitrectomy.
Dry Eye Syndrome
If your eyes are constantly itchy or dry, you may have dry eye syndrome, which affects many millions of Americans. Dry eye syndrome is caused by a lack of, or poor quality of, tears. Tears lubricate the outer layer of the eye called the cornea. If the tears are not adequate or are not composed of a proper balance of mucous, water, and oil, the eye becomes irritated.
Symptoms
Dry eye syndrome leads to a number of symptoms, including itchiness, irritation, burning, excessive tearing, redness, blurred vision that improves with blinking, and discomfort after long periods of watching television, using a computer, or reading.
Risk Factors
There are many factors that can contribute to dry eye syndrome. These include dry, hot, or windy climates; high altitudes; air-conditioned rooms; and cigarette smoke. Contact lens wearers, people with abnormally dry skin, and the elderly are more likely to develop dry eye syndrome. You may also be more at risk if you take certain medications, have a thyroid condition, a vitamin-A deficiency, Parkinson’s or Sjorgen’s disease, or if you are a woman going through menopause.
Glaucoma
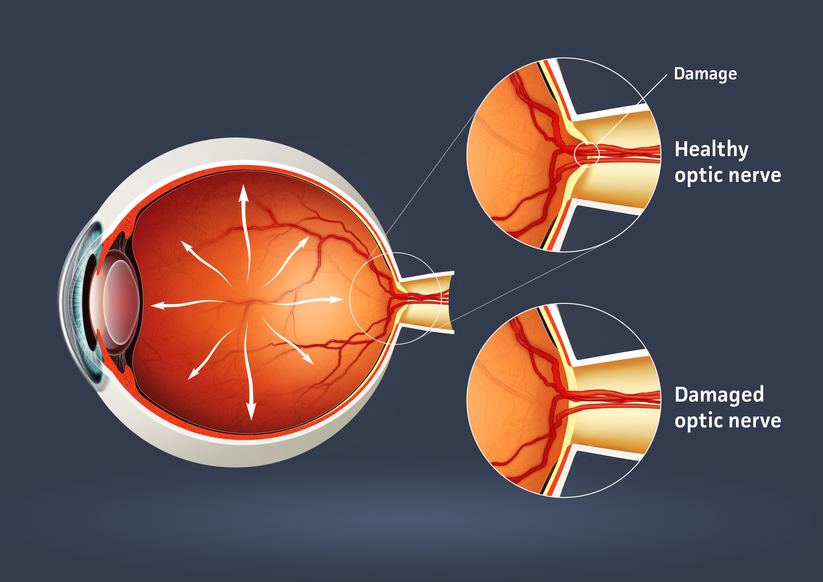
Glaucoma is a serious sight-threatening condition in which there is an abnormal pressure inside the eye. Typically, the pressure or IOP (intraocular pressure) is too high for the blood vessels and optic nerve to function normally, leading to loss of vision.
There are some forms of glaucoma that can occur with normal pressure in the eye. The average IOP for a healthy eye is 10 to 22 mm of Mercury. Just as a physician’s office tests your blood pressure annually, the eye doctor tests your IOP during annual eye examinations.
Types of Glaucoma
There are several varieties of the disease, with primary open-angle glaucoma being the most common. Primary open-angle glaucoma (POAG) occurs when the IOP is higher than normal. As the pressure increases, it destroys vital nerve tissue that is irreparable. POAG usually occurs over a long period of time, months to years, and slowly causes peripheral visual field loss. If left untreated, a sufferer progresses to tunnel vision and then to total blindness.
A second type of glaucoma is acute-angle closure. This is considered a medical emergency because the interocular pressure spikes suddenly to anywhere from 30-70 mm or higher. This causes extremely sharp pain, nausea and vomiting, and cloudy vision. The IOP needs to be lowered within hours to prevent permanent vision loss.
Juvenile open-angle glaucoma, or JOAP, is similar to POAG, in that is causes a gradual visual field loss. The most common form is in children from ages 3 to 21. Infantile or congenital glaucoma is a type of glaucoma that manifests itself between birth to 3 years of age. A typical sign is an enlarged bluish-gray cornea, the front dome of the eye. Excessive tearing of the eye and sensitivity to light are also symptoms. Finally, secondary glaucoma is caused from trauma, eye disease, or certain medications.
Causes of Glaucoma
Many theories on the cause of glaucoma exist, but the exact cause is unknown. Glaucoma can be a hereditary condition. It also can be caused by malformed anatomical structures in the eye. Certain risk factors such as hyperopia and cataracts cause a higher incidence of certain types of glaucoma.
One cause of glaucoma is an insufficient drainage system of the aqueous fluid. The aqueous imbalance causes a gradual buildup of pressure which destroys vision. Another cause is an insufficient flow of blood to the optic nerve. Ocular trauma or injury that damages the anterior segment for the lens and drainage mechanism of the eye can also lead to glaucoma. In the case of normal tension glaucoma, pressure readings are in the normal range. The cause of this is unknown.
Treatment
Even though in most cases there is no way to prevent glaucoma, there are many treatment options. Medications in the form of eyedrops are commonly prescribed. Different combinations of agents act on mechanisms of action to lower IOP or to slow the production of fluid.
Advanced surgical and laser procedures can also be viable options for the treatment of glaucoma. An in-office procedure called laser trabeculoplasty can cause the meshwork in the eye to work more efficiently. This treatment has a temporary effect and may need to be done multiple times. Another effective surgery uses a drainage implant to facilitate better outflow and inflow of aqueous fluid in the eye. These procedures help keep the pressure stabilized. Conventional surgery for glaucoma is done in an operating room scenario. A flap in the eye is created to facilitate outflow of the pressure. This pressure-controlling surgery is known as a trabeculotomy.
Furthermore, some oral medications can also be used in the treatment of glaucoma.
Methods of Testing for Glaucoma
During a comprehensive eye examination, eye pressure can be tested through various methods. Tonometry gives a pressure reading of the eye. A tomometer has different methods such as a probe that gently touches the front of the eye after the eye doctor has administered anesthetic eyedrops. Another method of testing uses a puff of air. For children, there is a tonometer that is quick and does not require anesthesia.
A pachometer, which measures the thickness of the front of the eye called the cornea, can also aid in diagnosis. A visual field device can measure for early or late damage in the peripheral fields of vision. Lastly, newer technology called OCT, or optical coherence tomography, counts the nerve fibers, which can help detect early changes in the disease.
Prevalence of Glaucoma
There are approximately 3 million individuals in the United States with glaucoma. It is the second leading cause of blindness in the country. Most cases are found in the population over age 40, and more women than men have the disease. Two thirds of glaucoma cases are in the Caucasian population, approximately 20% are African-American, and 10% are Hispanic. Glaucoma continues to rise every year in the population.
The key to success in the treatment of glaucoma is early detection and progressive monitoring of the condition. Comprehensive eye examinations and diligent monitoring will help protect from vision loss with this disease.
Citations
- Glaucoma. AOA pdf. AOA.org.
- I Care Tonometry in Children. JAAPOS. Sciencedirect.com. April 2011
- Glaucoma, open -angle. NEI source press release. 2010.
Macular Degeneration

Macular degeneration is a disease which affects a small area of the retina known as the macula. The macula is a specialized spot on the retina that allows us to see the fine detail of whatever is directly in front of us. Macular degeneration occurs when the macula begins to deteriorate.
“Wet” vs. “Dry”
Most often, macular degeneration is accompanied by formation of yellow deposits, called “drusen,” under the macula, which dry out or thin the macula. This is called “dry” macular degeneration. In rare cases, abnormal blood vessels develop under the macula and leak fluid. This is called “wet” macular degeneration.
Causes
A number of uncontrollable factors contribute to macular degeneration, including age, sex, eye color, farsightedness, and race. Risk factors you can control include smoking, high blood pressure, exposure to harmful sunlight, and diet.
Symptoms
It is difficult to detect dry macular degeneration in its early stages. The most common symptoms, when detected, include a spot of blurry vision, dark vision, or distorted vision. Wet macular degeneration progresses much faster than the dry variety. Both forms of macular degeneration can cause blindness.
Treatment
Currently, there is no cure for macular degeneration, but treatment is available to slow the effects.
Retinal Detachment
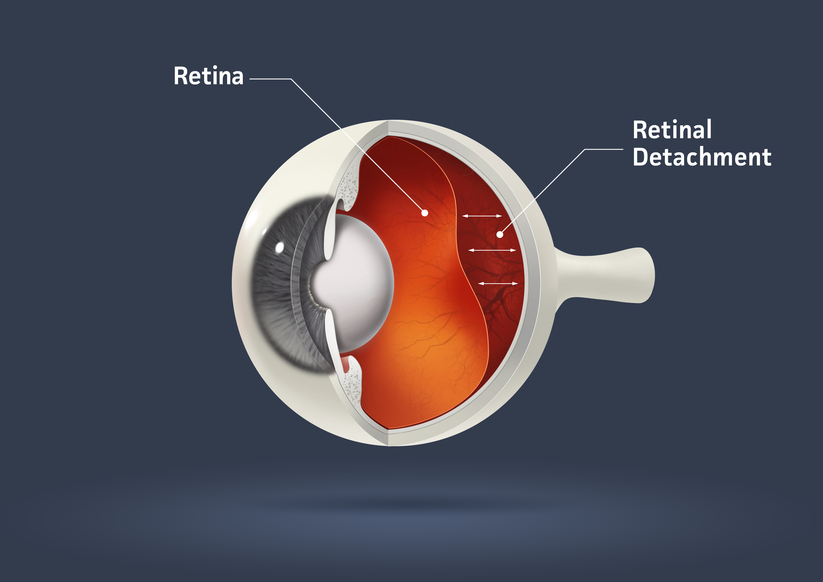
The part of the eye which collects light and transmits the light messages to the optic nerve and brain is the retina. It lines the inner back wall of the eye. When the retina separates from the back wall, it is known as retinal detachment. It is a serious condition which can cause permanent damage and vision loss if not treated quickly.
Symptoms
A retinal detachment often causes sudden defects in your vision. It may just cause a blind spot too small to notice, or it may cause a noticeable shadow which obscures your vision. An increase in “floaters,” which look like small particles or fine threads, may also be noticed. Finally, flashes of light are associated with retinal detachment.
Risk Factors
Eye injuries, tumors, and cataract surgery can cause retinal detachment. Nearsighted individuals and the elderly are at greater risk for spontaneous detachment. Also, diabetic retinopathy, a condition associated with diabetes, can cause bleeding which leads to retinal detachment.
Just for Presbyopes

Presbyopia is a Latin term for "old man eyes." This condition actually begins in your late 20s and slowly causes close vision loss. Most people develop symptoms after age 35--these symptoms include eyestrain and blurry vision while reading. Often presbyopia causes people to push objects further away to view them clearly. The treatment for presbyopia includes glasses and contact lenses, laser procedures, and other surgical procedures.
Reading glasses, bifocals, trifocals, or progressive multifocal blended lenses are all options to treat and correct presbyopia with glasses.
Soft, rigid, gas permeable, or a combination of these materials can treat presbyopia with contact lenses. Many surgical and laser techniques are used to treat presbyopia with new technology developing every year for this emerging population.
Computer Glasses
To reduce eye strain and fatigue, we carry specialized computer lenses. These lenses are perfect for computer users who spend a majority of their days working on computers. And since three out of four computer users will suffer from Computer Vision Syndrome, computer lenses are a great way to keep your eyesight healthy.
Reading Glasses
One of the first areas of your life where presbyopia becomes prominent is in your ability to read. There are a variety of styles available, with sleek designs that allow you to carry them anywhere.
No-Line Bifocals
For many presbyopes, bifocal lenses are a necessity. But it can be difficult to adjust to the harsh line that is found in many bifocal lenses. Fortunately, there are no-line lenses, which are also called progressive lenses. No more lines! Just a change in focusing power which allows you to comfortably focus on any distance. Just as with lined bifocals, distant objects are viewed through the top portion of the lenses, and near objects are viewed through the bottom portion of the lenses.
Bifocal Contacts
If you need bifocals but cannot stand wearing glasses, you may need bifocal contact lenses. Now you can have all of the benefits of bifocal lenses in the convenience of contact lenses. Talk with your doctor about bifocal contacts today.
Monovision Correction
For some of our emerging presbyopes we offer another option to glasses. Monovision is a method of fitting your dominant eye for distance vision and your non-dominant eye for near vision. Contacts are available in disposable, extended wear, and even daily disposable lenses to fit your lifestyle. Most patients require 2-4 weeks to make the adjustment from binocular vision to monovision.
Children's Vision
Children with uncorrected vision conditions or eye health problems face many barriers in life, academically, socially, and athletically. High-quality eye care can break down these barriers and help enable your children to reach their highest potential. As a parent, make sure you are giving your children the eye care they need. Presented are guidelines from the American Optometric Association.
Infant Vision

Your baby has a whole lifetime to see and learn. But did you know your baby also has to learn to see? As a parent, there are many things that you can do to help your baby’s vision develop.
When your baby is about six months, you should take him to your doctor of optometry for his first thorough eye examination. Things that the optometrist will test for include excessive or unequal amounts of nearsightedness, farsightedness, astigmatism, lack of eye movement ability, as well as other eye health problems. These problems are not common, but it is important to identify children who have them at this stage. Vision development and eye health problems can be more easily corrected if treatment is begun early.
Unless you notice a need, or your doctor of optometry advises you otherwise, your child’s next eye exam should be around age three, and then again before he or she enters school.
During the first four months of life, your baby should begin to follow moving objects with the eyes and to reach for things, first by chance and later more accurately, as hand-eye coordination and depth perception begin to develop.
To help, use a nightlight or other dim lamp in your baby’s room; change the crib’s position frequently and your child’s position in it; keep reach-and-touch toys within your baby’s focus, about eight to twelve inches from his eyes; talk to your baby as you walk around the room; alternate right and left sides with each feeding; and hang a mobile above and outside the crib.
Between four and eight months, your baby should begin to turn from side to side and use her arms and legs. Eye movement and eye/body coordination skills should develop further and both eyes should focus equally.
Enable your baby to explore different shapes and textures with his or her fingers; give your baby the freedom to crawl and explore; hang objects across the crib; and play “patty cake” and “peek-a-boo” with your baby.
From eight to twelve months, your baby should become mobile, crawling and pulling himself or herself up. He or she will begin to use both eyes together to judge distances and grasp and throw objects with greater precision. To support development do not encourage early walking – crawling is important in developing eye-hand-foot-body coordination; give your baby stacking and take-apart toys; and provide objects your baby can touch, hold and see at the same time.
From one to two years, your child’s eye-hand coordination and depth perception will continue to develop and he or she will begin to understand abstract terms. Things you can do are to encourage walking; to provide building blocks, simple puzzles and balls; and to provide opportunities to climb and explore indoors and out.
There are many other affectionate and loving ways in which you can aid your baby’s vision development. Use your creativity and imagination. Ask your doctor of optometry to suggest other specific activities.
Pre-School Vision

During the infant and toddler years, your child has been developing many vision skills and has been learning how to see. In the preschool years, this process continues as your child develops visually guided eye-hand-body coordination, fine motor skills, and the visual motor skills necessary to learn to read.
As a parent, you should watch for signs that may indicate a vision development problem, including a short attention span for the child’s age; difficulty with eye-hand-body coordination in ball play and bike riding; avoidance of coloring and puzzles and other detailed activities.
There are everyday things that you can do at home to help your preschooler’s vision develop as it should.
These activities include reading aloud to your child and letting him or her see what you are reading; providing a chalkboard, finger paints and different shaped blocks and showing your child how to use them in imaginative play; providing safe opportunities to use playground equipment such as a jungle gym and balance beam; and allowing time for interacting with other children and for playing independently.
By age three, your child should have a thorough optometric eye examination to make sure your preschooler’s vision is developing properly and there is no evidence of eye disease. If needed, your doctor can prescribe treatment including glasses and/or vision therapy to correct a vision development problem.
Here are several tips to make your child’s optometric examination a positive experience:
- Make an appointment early in the day. Allow about one hour.
- Talk about the examination in advance and encourage your child’s questions.
- Explain the examination in your child’s terms, comparing the E chart to a puzzle and the instruments to tiny flashlights and a kaleidoscope.
Unless recommended otherwise, your child’s next eye examination should be at age five. By comparing test results of the two examinations, your optometrist can tell how well your child’s vision is developing for the next major step. . .the school years.
School-Age Vision

A good education for your child means good schools, good teachers and good vision. Your child’s eyes are constantly in use in the classroom and at play. So when his or her vision is not functioning properly, learning and participation in recreational activities will suffer.
The basic vision skills needed for school use are:
- Near Vision. The ability to see clearly and comfortably at 10-13 inches.
- Distance Vision. The ability to see clearly and comfortably beyond arm’s reach.
- Binocular coordination. The ability to use both eyes together.
- Eye movement skills. The ability to aim the eyes accurately, move them smoothly across a page and shift them quickly and accurately from one object to another.
- Focusing skills. The ability to keep both eyes accurately focused at the proper distance to see clearly and the ability to change focus quickly.
- Peripheral awareness. The ability to be aware of things located to the side while looking straight ahead.
- Eye/hand coordination. The ability to use the eyes and hands together.
If any vision skills are lacking, your child will have to work harder. This can lead to headaches, fatigue, and other eyestrain problems. As a parent, be alert for symptoms that may indicate your child has a vision or visual processing problem. Be sure to tell your optometrist if your child frequently:
- Loses his place while reading.
- Avoids close work.
- Holds reading material closer than normal.
- Tends to rub his eyes.
- Has headaches.
- Turns or tilts head to use one eye only.
- Makes frequent reversals when reading or writing.
- Uses finger to maintain place when reading.
- Omits or confuses small words when reading.
- Consistently performs below potential.
Since vision changes can occur without you or your child noticing them, your child should visit the optometrist at least every two years, or more frequently if specific problems or risk factors exist. If needed, the doctor can prescribe treatment including eyeglasses, contact lenses, or vision therapy.
Remember, a school vision or pediatrician’s screening is not a substitute for a thorough eye examination.
Protective Eyewear

Never overlook the importance of safety eyewear when playing sports. Every year, hundreds of men, women, and children are injured while playing sports. To help prevent sports-related eye injuries, athletes should use protective athletic eyewear whether or not prescription eyewear is needed. One choice is a sports frame with prescription or non-prescription polycarbonate lenses. Baseball or softball players who are hit in or near the eye, or suffer a blow to the head, should seek immediate care at a hospital emergency room or from an eye care professional.
Children and Contact Lenses
The important thing to remember for parents of children who wear contact lenses is that contacts are prescribed medical devices. Contact lenses are not a cosmetic accessory. While the wearer may be happy about his or her new look, it is extremely important that the lenses be properly cleaned and worn according to the instructions of the optometrist.
Vision & Learning
- My Child Is Near-Sighted. Will Glasses Correct His/Her Learning Problem?
- What Is the Relationship between Eye Muscle Problems and Learning?
- My Child Loses His/Her Place. Is That Related to the Eyes?
- My Child Reverses Letters and Words. Does He See Backwards?
- What Are the Other Visual Components Necessary for Academic Achievement?
My Child Is Near-Sighted. Will Glasses Correct His/Her Learning Problem?

There is controversy over the exact relationship between vision and learning. For example there is a negative correlation between distance refractive error and reading ability. Myopic or nearsighted children who cannot see clearly at a distance without glasses are more commonly good readers. Children who spend tremendous amounts of time reading become nearsighted. Before Alaska became a state myopia was rare. After becoming a state, more than 50 percent of the children in Alaska developed nearsightedness. Thus, correlation is such that nearsightedness or poor distance vision is highly correlated with success in reading. Restated another way, poor distance vision is associated with better reading abilities. Farsighted children statistically are poorer readers than myopic children.
What Is the Relationship between Eye Muscle Problems and Learning?
Some of the mechanical visual skills which are related to reading include focusing or accommodation, and eye teaming, or convergence. Fatigue of one or both of these systems may interfere with reading. There is also a relationship between eye movements such as saccades (whereby we change fixation from one target to the next) and smooth following movements known as pursuits and reading. Children who cannot make accurate eye movements are often found to skip lines and words while reading.
The visual system was originally designed so that the peripheral vision was responsive to motion detection (danger from the jungles) with a central portion for fine discrimination (to identify the source of danger; e.g., a lion.) In the school environment the child is expected to ignore the peripheral portion of their visual system and pay attention with the central portion. If the child can not ignore the peripheral portion, he/she becomes distracted. Improvement in eye movement skills often results in less distraction and fewer errors of skipping words while reading.
My Child Loses His/Her Place. Is That Related to the Eyes?

Reading requires very accurate saccadics, which are fixations from one spot to another. Children who have poor eye movements are easily distracted and lose their place. Remember, the eye movement system was designed so that peripheral vision detects motion and danger. Imagine what happens when the system works correctly in the class room. As soon as there is peripheral movement, the eyes move toward the source of movement. This results in the complaint of inattention. Thus, reflexive eye movement skills must be socialized so that they do not respond reflexively to peripheral information. In addition, speed and accuracy must be trained so that one does not lose one’s place.
The skills are easily improvable with vision therapy. Once the information is brought into the eyes, it must be sent back to the brain for appropriate processing. The information must be utilized and integrated with the sensory and motor areas of the brain. Defects in the perceptual (interpretation of visual system) and motor (the integration with output, e.g., hand-eye coordination) may interfere with the reading process. Perceptual motor skills are key in the early acquisition of reading skills. A deficit is important to identify very early on-- i.e., five to seven years of age. Remediation of the skills at a later date, such as age 12, will be less effective for reading. Thus, early identification and treatment is essential. It is evident that there is more to good vision than 20/20.
My Child Reverses Letters and Words. Does He See Backwards?
It has been presumed that children who reverse letters or words see them backwards. This is false. They have directional confusion. In the real world direction has no meaning. For example, a chair is a chair no matter which way it is placed. Changing direction does not change interpretation. In the world of language direction changes meaning. Connect the bottom of a chair and it looks like a "b". Turn it 180 degrees it becomes a "d", flip it upside down and it becomes a "q" and flip it again it becomes a "p". Thus, direction changes meaning. The difference between "was" and "saw" is direction.
What Are the Other Visual Components Necessary for Academic Achievement?
As mentioned previously, we should correct all optical errors of the eyes (glasses); eliminate eye muscle problems; and create smooth accurate eye movements. In addition, we should make sure that we properly interpret what we see and use it appropriately. These are known collectively as perceptual skills and include form perception, size and shape recognition, visual memory, and visual motor integration (hand-eye coordination.)
To See Clearly, Get Checked Yearly.
 Truly Comprehensive Care
Truly Comprehensive Care
Our office philosophy is that no exam is "routine." Instead, every comprehensive examination performed in our office is tailored to your specific concerns and needs. Your visual system will be analyzed, and your eye health thoroughly evaluated. Dr. Baker prides himself in his discussion and summary of your eyes and vision, and aims to have individuals leave as well-informed patients.
Treatment of Eye and Vision Diseases
Dr. Baker and staff are highly trained to manage a number of eye conditions, both treatable and untreatable, inherited and acquired (or age-related). Cataracts. glaucoma, macular degeneration, diabetes complications, dry eye, and more are encountered daily. In advanced cases, Dr. Baker works closely with area specialists and surgeons to best manage your care.
Urgent Eyecare and Emergency Services
Our office is equipped to handle injuries, infections, new-onset issues swiftly and effectively. We want to get you feeling better and back to your normal routine as soon as possible. Our office is available on a 24-hour basis for true eye emergencies. Chemical splashes to the eye, injuries to the eye and eyelids, and potential infections should be addressed immediately. Please contact 428-2526 for more information.
Eyewear
Our office has over 800 frames on display in a wide variety of styles and fashion. We offer numerous designer frame lines and only use the industry's best warranties. Our staff is well prepared to help you select an attractive frame while providing information on lens features that will also improve vision and performance.
Contact Lenses
Contact lenses are a great option for nearly all patients. Your contact lens type and brand will be carefully chosen by Dr. Baker to suit your visual and lifestyle needs. Contact Lenses can be worn for nearly any prescription (including astigmatism and bifocal wearers). Of course, proper lens care and safety will be critical to a healthy eye. Dr. Baker will discuss the specifics of your particular lens to best avoid any complications.
Surgical Co-Management
Dr. Baker works closely with numerous area surgeons to perform peri-operative care management for glaucoma surgery, cataract surgery, and refractive surgery (including LASIK).
How Often Do I Need an Exam?
| Here's a general guideline: | Infants 6 month - 1 Year | First Exam (InfantSEE) |
| Age 3 to 5 years | Every 2 years | |
| Age 6 to 18 years (school-age) | Yearly or every 2 years | |
| Age 18 to 60 years | Every 2 years | |
| Over age 60 | Yearly |
Of course, every person has different needs. Your eye history and medical history play a large role.
| Yearly exams are required for: |
|
|
|
More frequent eye exams may be required in special circumstances of illness or disease.
Dr. Baker will inform you when you should be regularly examined.
Comprehensive Eyecare

Truly Comprehensive Care
Our office philosophy is that no exam is "routine." Instead, every examination performed in our office is tailored to your specific concerns and needs.
Wellness Exams for Eyeglasses, Contact Lenses, and Refractive Surgery
Your care starts with basics - getting you to see your best and checking for abnormalities. Your visual system will be analyzed, and your eye health thoroughly evaluated. Dr. Baker prides himself in his discussion and summary of your eyes and vision, and aims to have individuals leave as well-informed patients. Read more about routine wellness visits here.
Treatment of Eye and Vision Diseases
Dr. Baker and staff are highly trained to manage a number of eye conditions, both treatable and untreatable, inherited and acquired (or age-related). Cataracts. glaucoma, macular degeneration, diabetes complications, dry eye, and more are encountered daily. In advanced cases, Dr. Baker works closely with area specialists and surgeons to best manage your care.
Urgent Eyecare and Emergency Services
Our office is equipped to handle injuries, infections, new-onset issues swiftly and effectively. We want to get you feeling better and back to your normal routine as soon as possible. Our office is available on a 24-hour basis for true eye emergencies. Chemical splashes to the eye, injuries to the eye and eyelids, and potential infections should be addressed immediately. Please contact 428-2526 for more information.
Eyewear
Our office has over 800 frames on display in a wide variety of styles and fashion. We offer numerous designer frame lines and only use the industry's best warranties. Our staff is well prepared to help you select an attractive frame while providing information on lens features that will also improve vision and performance.
Contact Lenses
Contact lenses are a great option for nearly all patients. Your contact lens type and brand will be carefully chosen by Dr. Baker to suit your visual and lifestyle needs. Contact Lenses can be worn for nearly any prescription (including astigmatism and bifocal wearers). Of course, proper lens care and safety will be critical to a healthy eye. Dr. Baker will discuss the specifics of your particular lens to best avoid any complications.
Surgical Co-Management
Dr. Baker works closely with numerous area surgeons to perform peri-operative care management for glaucoma surgery, cataract surgery, and refractive surgery (including LASIK).
How Often Do I Need an Exam?
| Here's a general guideline: | Infants 6 month - 1 Year | First Exam (InfantSEE) |
| Age 3 to 5 years | Every 2 years | |
| Age 6 to 18 years (school-age) | Yearly or every 2 years | |
| Age 18 to 60 years | Every 2 years | |
| Over age 60 | Yearly |
Of course, every person has different needs. Your eye history and medical history play a large role.
| Yearly exams are required for: |
|
|
|
More frequent eye exams may be required in special circumstances of illness or disease.
Dr. Baker will inform you when you should be regularly examined.
Widefield Retinal Imaging
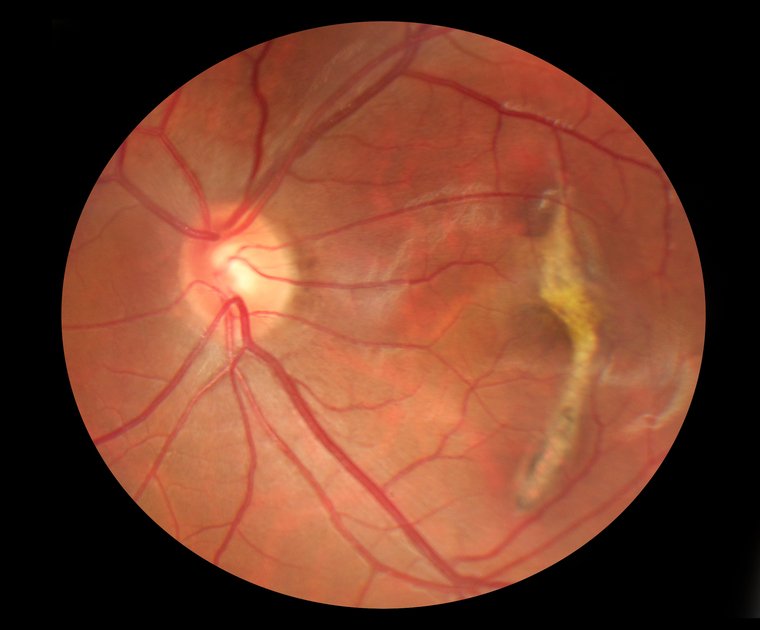
In our continued efforts to bring the most advanced technology available to our patients, Dr. Baker is proud to announce the inclusion of the digital widefield retinal imaging as an integral part of your eye exam. This has been a tremendous resource and Dr. Baker now views it as a necessity for thorough care.
Many eye problems can develop without warning and progress with no symptoms. Early on, you might not notice any change in your vision. However, diseases such as macular degeneration, glaucoma, retinal tears or detachments, as well as other health problems such as diabetes and high blood pressure, can often be detected with a thorough exam of the retina. The retina is the part of your eye that catches the image of what you are looking at, similar to the film in a camera.
Digital widefield retinal imaging provides:
- A scan to confirm a healthy eye or detect the presence of disease.
- An overview or map of the retina, giving your eye doctor a more complete view than he can achieve by other means.
- The opportunity for you to view and discuss the retinal images of your eye with your doctor at the time of your exam.
- A permanent record for your medical file, enabling your doctor to make important comparisons if potential problems show themselves at a future examination.
Widefield Retinal Imaging

In our continued efforts to bring the most advanced technology available to our patients, Dr. Baker is proud to announce the inclusion of the digital widefield retinal imaging as an integral part of your eye exam. This has been a tremendous resource and Dr. Baker now views it as a necessity for thorough care.
Many eye problems can develop without warning and progress with no symptoms. Early on, you might not notice any change in your vision. However, diseases such as macular degeneration, glaucoma, retinal tears or detachments, as well as other health problems such as diabetes and high blood pressure, can often be detected with a thorough exam of the retina. The retina is the part of your eye that catches the image of what you are looking at, similar to the film in a camera.
Digital widefield retinal imaging provides:
- A scan to confirm a healthy eye or detect the presence of disease.
- An overview or map of the retina, giving your eye doctor a more complete view than he can achieve by other means.
- The opportunity for you to view and discuss the retinal images of your eye with your doctor at the time of your exam.
- A permanent record for your medical file, enabling your doctor to make important comparisons if potential problems show themselves at a future examination.
Dr. Michael A. Baker, O.D. - Optometrist

Dr. Michael A. Baker, O.D. - Optometrist
Doctor Baker proudly returned to his hometown of Madison to join the practice of his own childhood optometrist, Doctor Nick Donch. Doctor Baker earned his optometry degree from The Ohio State University following a bachelor’s degree from the University of Toledo. He had trained at the Hampton Virginia Veteran’s Hospital as well as a prestigious cataract and glaucoma surgical office in central Pennsylvania. Dr. Baker is a member of the American Optometric Association and the Ohio Optometric Association.
Dr. Baker has established our in-office Dry Eye Clinic as well as expanded our Glaucoma Service to reflect his interest in those two conditions. He also takes pride in fitting multifocal contact lenses, managing digital eye strain and computer vision syndrome, and evaluating pediatric patients.
Dr. Baker lives in Hartsgrove with his wife Kelli and four children.
Laurie – Licensed Optician

Laurie – Licensed Optician
With 30 years of knowledge and experience, Laurie offers a level of expertise unique to our office. Between her technical knowledge of ophthalmic lens designs and understanding of available lens improvements and treatments, her simple goal to help everyone see their best out of their new glasses prescription. Most importantly, Laurie only recommends what can truly make a difference– nothing unnecessary.
Laurie understands prescription eyeglasses are also a hybrid of function and fashion and is always on the lookout for new styles or recommendations for our patients.
Nicole – Certified Paraoptometric

Nicole – Certified Paraoptometric
Nicole is our primary patient care assistant and will often begin your examination by performing some tests and obtaining your health information. She oversees our ancillary testing as well, performing tests requested by Dr. Baker to better evaluate patient's conditions. She very quickly has absorbed a wealth of information and is eager to grow with our office to help our patients receive the best possible care. She is a certified paraoptometric.
Nicole also has a hand in preparing insurance documents prior to your arrival to help understand what tests, procedures, and items may and may not be covered. No one likes surprises after all.
Like Dr. Baker, Nicole is also a born-and-bred Madison local. Nicole has become Dr. Baker’s go-to for translating youthful slang to make him SO WOKE.
Deanna - Patient Care Coordinator

Deanna - Patient Care Coordinator
As our full-time Patient Care Coordinator, Deanna handles many of the day to day managerial aspects of the office in addition to her front desk reception duties. From the time you call our office to schedule your exam, to the moment your visit is complete, Deanna ensures you are properly cared for. She is happy to answer any questions, and never hesitates to provide unsurpassed customer service. With Deanna’s help, our patients experience a seamless visit with a personal touch.
Deanna is our easy-going, fun-loving teammate that makes coming to the office a true pleasure. She and her husband Victor have raised five kids, all Madison and college graduates. Although she’s a northeast Ohio native, she has a deep love for Holmes County and believes she has a spiritual connection to Janis Joplin (or at least that’s what Dr. Baker calls it).
Carolyn – Reception

Carolyn – Reception
Helping out part-time, Carolyn is often the first to pick up the telephone and tend to your needs. She is remarkably thorough and is phenomenal to anticipate the “other questions” that might come up as we prepare for your visit. Dr. Baker says she “connects the dots” between a patient and their insurance better than anyone – knowing what information might be needed to obtain the care you need.
Carolyn and her husband Steve are longtime Lake County residents, recently building a new home in Perry; complete with rooms for the grandkids when they come to stay.
JoAnn – Treasurer and Insurance Adjudicator

JoAnn – Treasurer and Insurance Adjudicator
JoAnn oversees many of the operational aspects of the office and is much appreciated for her dedication to the practice from even before Dr. Baker took leadership. She works behind the scenes to coordinate with insurance companies to assure your coverage and benefits are properly utilized. With JoAnn's help, our office runs smoothly and efficiently.
JoAnn enjoys swimming, fine arts, and traveling. Favorite destinations include the Caribbean, European river cruises, China, and even the Antarctic circle.
Dr. Nick J. Donch, O.D. - Optometrist (Emeritus)

Dr. Nick J. Donch, O.D. - Optometrist (Emeritus)
For 46 years, Doctor Donch served and examined the Madison community. Dr. Donch had visited both Honduras and Siberia to perform volunteer eye examinations in those underserved areas.
Dr. Donch and JoAnn, his wife of 47 years, have been proud to call Madison home. Together, they have two daughters Sherry and Diana. Some of our patients may remember Dr. Diana as she practiced optometry in her father’s Madison office prior to establishing her own practice in Pennsylvania.
Dr. Donch passed away in June 2011, but as his mentor, Dr. Baker still leaves his profile up in fond memory.